Refractive error
| Refractive error | |
|---|---|
| Other names | Refraction error |
 | |
| A correctly-focused eye (top), and two showing refractive error: in the middle image, the light is focused too far forward; in the bottom image, the focal point is behind the eye | |
| Specialty | Ophthalmology, optometry |
| Symptoms | Blurry vision, double vision, headaches, eye strain |
| Complications | Blindness, amblyopia[1][2] |
| Types | Near-sightedness, far-sightedness, astigmatism, presbyopia[3] |
| Causes | Eyeball length, problems with cornea shape, aging of the lens[3] |
| Diagnostic method | Eye examination[3] |
| Treatment | Eyeglasses, contact lenses, refractive surgery[3] |
| Frequency | ~1.5 billion[4] |
Refractive error is a problem with focusing light accurately on the retina due to the shape of the eye and/or cornea.[3] The most common types of refractive error are near-sightedness, far-sightedness, astigmatism, and presbyopia. Near-sightedness results in far away objects being blurry, far-sightedness and presbyopia result in close objects being blurry, and astigmatism causes objects to appear stretched out or blurry. Other symptoms may include double vision, headaches, and eye strain.[3]
Near-sightedness is due to the length of the eyeball being too long, far-sightedness the eyeball too short, astigmatism, the cornea being the wrong shape, and presbyopia aging of the lens of the eye such that it cannot change shape sufficiently.[3] Some refractive errors occur more often among those whose parents are affected. Diagnosis is by eye examination.
Refractive errors are corrected with eyeglasses, contact lenses, or surgery.[3] Eyeglasses are the easiest and safest method of correction. Contact lenses can provide a wider field of vision; however they are associated with a risk of infection. Refractive surgery permanently changes the shape of the cornea.[3]
The number of people globally with refractive errors has been estimated at one to two billion.[4] Rates vary between regions of the world with about 25% of Europeans and 80% of Asians affected.[4] Near-sightedness is the most common disorder.[5] Rates among adults are between 15 and 49% while rates among children are between 1.2 and 42%.[6] Far-sightedness more commonly affects young children and the elderly.[7][8] Presbyopia affects most people over the age of 35.[3]
The number of people with refractive errors that have not been corrected was estimated at 660 million (10 per 100 people) in 2013.[9] Of these 9.5 million were blind due to the refractive error.[9] It is one of the most common causes of vision loss along with cataracts, macular degeneration, and vitamin A deficiency.[10]
Classification
[edit]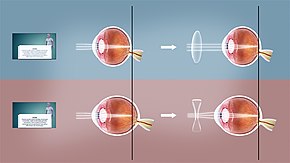
Refractive error – sometimes called "ametropia" – is when the refractive power of an eye does not match the length of the eye, so the image is focused away from the central retina, instead of directly on it.[11][12]
Types of refractive error include myopia, hyperopia, presbyopia, and astigmatism.
- Myopia or Nearsightedness: When the refractive power is too strong for the length of the eyeball, this is called myopia or nearsightedness. People with myopia typically have blurry vision when viewing distant objects because the eye is refracting more than necessary. Myopia can be corrected with a concave lens, which causes the divergence of light rays before they reach the cornea.[citation needed]
- Hyperopia or Farsightedness: When the refractive power is too weak for the length of the eyeball, one has hyperopia or farsightedness. People with hyperopia have blurry vision when viewing near objects because the eye is unable to focus the light sufficiently. This can be corrected with convex lenses, which cause light rays to converge prior to hitting the cornea.[13]
- Presbyopia: When the flexibility of the lens declines, typically due to age. The individual would experience difficulty in near vision, often relieved by reading glasses, bifocal, or progressive lenses.[14]
- Astigmatism is when the refractive power of the eye is not uniform across the surface of the cornea because of asymmetry. In other words, the eye focuses light more strongly in one direction than another, leading to distortion of the image.[15]
Children are typically born hyperopic and shift toward emmetropia or myopia as their eyes lengthen through childhood.[16]
Other terminology include anisometropia, when the two eyes have unequal refractive power,[17] and aniseikonia which is when the magnification power between the eyes differ.[18]
Refractive errors are typically measured using three numbers: sphere, cylinder, and axis.[19]
- Sphere: This number denotes the strength of the lens needed to correct your vision. A "–" indicates nearsightedness while a "+" indicates farsightedness. Higher numbers indicate more power in either direction.
- Cylinder: This number denotes the amount of astigmatism, if any.
- Axis: This number notes the direction of the astigmatism and is written in degrees between 1 and 180.
An eye that has no refractive error when viewing distant objects is said to have emmetropia or be emmetropic meaning the eye is in a state in which it can focus parallel rays of light (light from distant objects) on the retina, without using any accommodation. A distant object, in this case, is defined as an object located beyond 6 meters, or 20 feet, from the eye, since the light from those objects arrives as essentially parallel rays when considering the limitations of human perception.[20]
Risk factors
[edit]Genetics
[edit]
There is evidence to suggest genetic predilection for refractive error. Individuals that have parents with certain refractive errors are more likely to have similar refractive errors.[3]
The Online Mendelian Inheritance in Man (OMIM) database has listed 261 genetic disorders in which myopia is one of the symptoms.[21] Myopia may be present in heritable connective tissue disorders such as: Knobloch syndrome (OMIM 267750); Marfan syndrome (OMIM 154700); and Stickler syndrome (type 1, OMIM 108300; type 2, OMIM 604841).[22] Myopia has also been reported in X-linked disorders caused by mutations in loci involved in retinal photoreceptor function (NYX, RP2, MYP1) such as: autosomal recessive congenital stationary night blindness (CSNB; OMIM 310500); retinitis pigmentosa 2 (RP2; OMIM 312600); Bornholm eye disease (OMIM 310460).[22] Many genes that have been associated with refractive error are clustered into common biological networks involved in connective tissue growth and extracellular matrix organization.[22] Although a large number of chromosomal localisations have been associated with myopia (MYP1-MYP17), few specific genes have been identified.[21]
Environmental
[edit]In studies of the genetic predisposition of refractive error, there is a correlation between environmental factors and the risk of developing myopia.[23] Myopia has been observed in individuals with visually intensive occupations.[22] Reading has also been found to be a predictor of myopia in children. It has been reported that children with myopia spent significantly more time reading than non-myopic children who spent more time playing outdoors.[22] Additionally, focusing on near objects for long periods of time - such as when reading, looking at close screens, or writing - has been associated with myopia.[24][25] Socioeconomic status and higher levels of education have also been reported to be a risk factor for myopia.[26] Blepharoptosis can also induce refractive errors.[27]
Normal Refraction
[edit]In order to see a clear image, the eye must focus rays of light on to the light-sensing part of the eye – the retina, which is located in the back of the eye. This focusing – called refraction – is performed mainly by the cornea and the lens, which are located at the front of the eye, the anterior segment.[28]
When an eye focuses light correctly on to the retina when viewing distant objects, this is called emmetropia or being emmetropic. This means that the refractive power of the eye matches what is needed to focus parallel rays of light onto the retina. A distant object is defined as an object located beyond 6 meters (20 feet) from the eye.[citation needed]
When an object is located close to the eye, the rays of light from this object no longer approach the eye parallel to each other. Consequently, the eye must increase its refractive power to bring those rays of light together on the retina. This is called accommodation, and is accomplished by the eye thickening the lens.[28]
Diagnosis
[edit]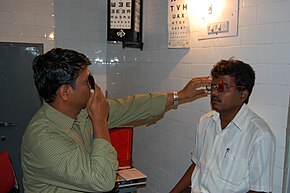
Blurry vision may result from any number of conditions not necessarily related to refractive errors. The diagnosis of a refractive error is usually confirmed by an eye care professional during an eye examination using a large number of lenses of different optical powers, and often a retinoscope (a procedure entitled retinoscopy) to measure objectively in which the person views a distant spot while the clinician changes the lenses held before the person's eye and watches the pattern of reflection of a small light shone on the eye. Following that "objective refraction" the clinician typically shows the person lenses of progressively higher or weaker powers in a process known as subjective refraction. Cycloplegic agents are frequently used to more accurately determine the amount of refractive error, particularly in children[23]
An automated refractor is an instrument that is sometimes used in place of retinoscopy to objectively estimate a person's refractive error.[29] Shack–Hartmann wavefront sensor and its inverse[30] can also be used to characterize eye aberrations in a higher level of resolution and accuracy.
Vision defects caused by refractive error can be distinguished from other problems using a pinhole occluder, which will improve vision only in the case of refractive error.[31]
Screening
[edit]When refractive errors in children are not treated, the child may be at risk of developing ambylopia, where vision may remain permanently blurry.[32] Because young children typically do not complain of blurry vision, the American Academy of Pediatrics recommends that children have yearly vision screening starting at three years old so that unknown refractive errors or other ophthalmic conditions can be found and treated if deemed necessary by healthcare professionals.[32][33]
Management
[edit]The management of refractive error is done post-diagnosis of the condition by either optometrists, ophthalmologists, refractionists, or ophthalmic medical practitioners.[34]
How refractive errors are treated or managed depends upon the amount and severity of the condition. Those who possess mild amounts of refractive error may elect to leave the condition uncorrected, particularly if the person is asymptomatic. For those who are symptomatic, glasses, contact lenses, refractive surgery, or a combination are typically used.[28][19][21]
Glasses
[edit]These are the most effective ways of correcting the refractive error. However, the availability and affordability of eyeglasses can present a difficulty for people in many low income settings of the world. Glasses also pose a challenge to children to whom they are prescribed to, due to children's tendency to not wear them as consistently as recommended.[35]
As mentioned earlier refractive errors are because of the improper focusing of the light in the retina. Eyeglasses work as an added lens of the eye serving to bend the light to bring it to focus on the retina. Depending on the eyeglasses, they serve many functions.[36]
- Reading glasses
- These are general over-the-counter glasses which can be worn for easier reading, especially for defective vision due to aging called presbyopia.
- Single vision prescription lenses
- They can correct only one form of defective vision, either far-sightedness or near-sightedness.
- Multifocal lenses
- The multifocal lenses can correct defective vision in multiple focus, for example: near-vision as well as far-vision. This are particularly beneficial for presbyobia.[37]
Contact lenses
[edit]Alternatively, many people choose to wear contact lenses. One style is hard contact lenses, which can distort the shape of the cornea to a desired shape. Another style, soft contact lenses, are made of silicone or hydrogel. Depending on the duration they are designed for, they may be worn daily or may be worn for an extended period of time, such as for weeks.[34]
There are a number of complication associated with contact lenses. Typically the ones that are used daily.[citation needed]
| Complications of contact lens wear | Description |
|---|---|
| Conjunctivitis (giant papillary form) | Caused in response to the allergen present in the material from which the contact lens is made from. There is often discomfort in the eye after wearing and vision may be affected. Choosing the right lens material and changing it regularly might prevent conjunctivitis. |
| Corneal abrasion | Caused by a foreign body, dust, sand, or grit trapped under the lens. |
| Corneal edema | Caused by decreased oxygen delivery to the tissue compressed by the lens. Usually resolved after the removal of the lenses. Discomfort upon lens removal may be seen. |
| Neovascularization | New blood vessels may form in the iris region and the limbus. This may impair vision. |
| Infections | Various viral, bacterial, and fungal infection may be seen in the eye post-contact-lens wear, if proper lens hygiene is not maintained. Acanthamoeba are the most common infections in the people using contact lenses. |
If redness, itching, and difficulty in vision develops, the use of the lenses should be stopped immediately and the consultation of ophthalmologists may be sought.
Surgery
[edit]Laser in situ keratomileusis (LASIK) and photo-refractive keratectomy (PRK) are popular procedures; while use of laser epithelial keratomileusis (LASEK) is increasing. Other surgical treatments for severe myopia include insertion of implants after clear lens extraction (refractive lens exchange). Full thickness corneal graft may be a final option for patients with advanced kerataconus although currently there is interest in new techniques that involve collagen crosslinking. As with any surgical procedure complications may arise post-operatively Post-operative monitoring is normally undertaken by the specialist ophthalmic surgical clinic and optometry services. Patients are usually informed pre-operatively about what to expect and where to go if they suspect complications. Any patient reporting pain and redness after surgery should be referred urgently to their ophthalmic surgeon.[38][39]
Medical treatment
[edit]Atropine has believed to slow the progression of near-sightedness and is administered in combination with multifocal lenses. These, however, need further research.[40][41]
Prevention
[edit]Strategies being studied to slow worsening include adjusting working conditions, increasing the time children spend outdoors,[22] and special types of contact lenses.[42] In children special contact lenses appear to slow worsening of nearsightedness.[42][43]
A number of questionnaires exist to determine quality of life impact of refractive errors and their correction.[44][45]
Epidemiology
[edit]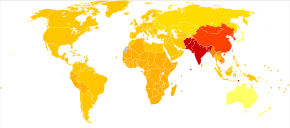
It is estimated that at least 2 billion people in the world have refractive errors.[4] The number of people globally with refractive errors that have not been corrected was estimated at 660 million (10 per 100 people) in 2013.[9]
Refractive Errors are the first common cause of Visual Impairment and second most common cause of visual loss .[47] The assessment of Refractive Error is now done in DALY (Disability Adjusted Life Years) which showed an 8% increase from 1990 to 2019.[48][unreliable source]
The number of people globally with significant refractive errors has been estimated at one to two billion.[4] Rates vary between regions of the world with about 25% of Europeans and 80% of Asians affected.[4] Near-sightedness is one of the most prevalent disorders of the eye.[5] Rates among adults are between 15 and 49% while rates among children are between 1.2 and 42%.[6] Far-sightedness more commonly affects young children, whose eyes have yet to grow to their full length, and the elderly, who have lost the ability to compensate with their accommodation system.[7][8] Presbyopia affects most people over the age of 35, and nearly 100% of people by the ages of 55–65.[3] Uncorrected refractive error is responsible for visual impairment and disability for many people worldwide.[9] It is one of the most common causes of vision loss along with cataracts, macular degeneration, and vitamin A deficiency.[10]
Cost
[edit]The yearly cost of correcting refractive errors is estimated at 3.9 to 7.2 billion dollars in the United States.[49]
References
[edit]- ^ "Care of the Patient with Amblyopia" (PDF). Archived from the original (PDF) on 19 August 2016. Retrieved 17 February 2020.
- ^ Dandona, R; Dandona, L (2001). "Refractive error blindness". Bulletin of the World Health Organization. 79 (3): 237–43. PMC 2566380. PMID 11285669.
- ^ a b c d e f g h i j k l "Facts About Refractive Errors". NEI. October 2010. Archived from the original on 28 July 2016. Retrieved 29 July 2016.
- ^ a b c d e f Denniston, Alastair; Murray, Philip (2018). Oxford Handbook of Ophthalmology (4 ed.). OUP Oxford. p. 926. ISBN 9780198816751.
- ^ a b Foster, PJ; Jiang, Y (February 2014). "Epidemiology of myopia". Eye. 28 (2): 202–8. doi:10.1038/eye.2013.280. PMC 3930282. PMID 24406412.
- ^ a b Pan, CW; Ramamurthy, D; Saw, SM (January 2012). "Worldwide prevalence and risk factors for myopia". Ophthalmic & Physiological Optics. 32 (1): 3–16. doi:10.1111/j.1475-1313.2011.00884.x. PMID 22150586. S2CID 32397628.
- ^ a b Castagno, VD; Fassa, AG; Carret, ML; Vilela, MA; Meucci, RD (23 December 2014). "Hyperopia: a meta-analysis of prevalence and a review of associated factors among school-aged children". BMC Ophthalmology. 14: 163. doi:10.1186/1471-2415-14-163. PMC 4391667. PMID 25539893.
- ^ a b Grosvenor, Theodore (2007). Primary care optometry (5 ed.). St. Louis (Miss.): Butterworth Heinemann, Elsevier. p. 70. ISBN 9780750675758. Archived from the original on 2016-08-15.
- ^ a b c d Vos, Theo; Barber, Ryan M; Bell, Brad; Bertozzi-Villa, Amelia; Biryukov, Stan; Bolliger, Ian; et al. (Global Burden of Disease Study 2013 Collaborators) (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 386 (9995): 743–800. doi:10.1016/s0140-6736(15)60692-4. PMC 4561509. PMID 26063472.
- ^ a b Pan, CW; Dirani, M; Cheng, CY; Wong, TY; Saw, SM (March 2015). "The age-specific prevalence of myopia in Asia: a meta-analysis". Optometry and Vision Science. 92 (3): 258–66. doi:10.1097/opx.0000000000000516. PMID 25611765. S2CID 42359341.
- ^ Lawrenson, John G; Shah, Rakhee; Huntjens, Byki; Downie, Laura E; Virgili, Gianni; Dhakal, Rohit; Verkicharla, Pavan K; Li, Dongfeng; Mavi, Sonia; Kernohan, Ashleigh; Li, Tianjing; Walline, Jeffrey J (2023-02-16). Cochrane Eyes and Vision Group (ed.). "Interventions for myopia control in children: a living systematic review and network meta-analysis". Cochrane Database of Systematic Reviews. 2023 (2): CD014758. doi:10.1002/14651858.CD014758.pub2. PMC 9933422. PMID 36809645.
- ^ Walline, Jeffrey J; Lindsley, Kristina B; Vedula, S Swaroop; Cotter, Susan A; Mutti, Donald O; Ng, Sueko M; Twelker, J. Daniel (2020-01-13). Cochrane Eyes and Vision Group (ed.). "Interventions to slow progression of myopia in children". Cochrane Database of Systematic Reviews. 2021 (9): CD004916. doi:10.1002/14651858.CD004916.pub4. PMC 6984636. PMID 31930781.
- ^ Grosvenor, Theodore (2007). Primary care optometry (5 ed.). St. Louis (Miss.): Butterworth Heinemann, Elsevier. p. 17. ISBN 9780750675758.
- ^ Khurana, AK (September 2008). "Asthenopia, anomalies of accommodation and convergence". Theory and practice of optics and refraction (2nd ed.). Elsevier. pp. 100–103. ISBN 978-81-312-1132-8.
- ^ Grosvenor, Theodore (2007). Primary care optometry (5 ed.). St. Louis (Miss.): Butterworth Heinemann, Elsevier. pp. 17–19. ISBN 9780750675758.
- ^ Saluja, Gunjan; Kaur, Kirandeep (2023), "Childhood Myopia and Ocular Development", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 36508524, retrieved 2023-10-31
- ^ "Anisometropia - American Association for Pediatric Ophthalmology and Strabismus". aapos.org. Retrieved 10 February 2020.
- ^ "Aniseikonia - EyeWiki". eyewiki.aao.org. Retrieved 10 February 2020.
- ^ a b Porter, Daniel (2023-04-18). "How to Read an Eyeglasses Prescription". American Academy of Ophthalmology. Retrieved 2023-10-31.
- ^ Bope, Edward T.; Kellerman, Rick D. (2015). Conn's Current Therapy 2016. Elsevier Health Sciences. p. 354. ISBN 9780323355353.
- ^ a b c Morgan, Ian; Kyoko Ohno-Matsui (May 2012). "Myopia". The Lancet. 379 (9827): 1739–1748. doi:10.1016/S0140-6736(12)60272-4. PMID 22559900. S2CID 208793136.
- ^ a b c d e f Wojciechowski, Robert (April 2011). "Nature and Nurture: the complex genetics of myopia and refractive error". Clinical Genetics. 79 (4): 301–320. doi:10.1111/j.1399-0004.2010.01592.x. PMC 3058260. PMID 21155761.
- ^ a b Barnes, Katherine (Feb 2013). "Genome-wide meta-analyses of multiancestry cohorts identify multiple new susceptibility loci for refractive error and myopia". Clinical Genetics. 45 (3): 314–8. doi:10.1111/j.1399-0004.2010.01592.x. PMC 3740568. PMID 23396134.
- ^ Huang, Hsiu-Mei; Chang, Dolly Shuo-Teh; Wu, Pei-Chang (2015-10-20). Jhanji, Vishal (ed.). "The Association between Near Work Activities and Myopia in Children—A Systematic Review and Meta-Analysis". PLOS ONE. 10 (10): e0140419. Bibcode:2015PLoSO..1040419H. doi:10.1371/journal.pone.0140419. ISSN 1932-6203. PMC 4618477. PMID 26485393.
- ^ Dutheil, Frédéric; Oueslati, Tharwa; Delamarre, Louis; Castanon, Joris; Maurin, Caroline; Chiambaretta, Frédéric; Baker, Julien S.; Ugbolue, Ukadike C.; Zak, Marek; Lakbar, Ines; Pereira, Bruno; Navel, Valentin (2023-01-03). "Myopia and Near Work: A Systematic Review and Meta-Analysis". International Journal of Environmental Research and Public Health. 20 (1): 875. doi:10.3390/ijerph20010875. ISSN 1660-4601. PMC 9820324. PMID 36613196.
- ^ Foster, P J; Jiang, Y (February 2014). "Epidemiology of myopia". Eye. 28 (2): 202–208. doi:10.1038/eye.2013.280. ISSN 0950-222X. PMC 3930282. PMID 24406412.
- ^ Owji, N; Khalili, MR; Bazrafkan, H; Heydari, M (September 2022). "Long-term outcome of refractive errors in patients with congenital blepharoptosis who have undergone ptosis surgery". Clinical & Experimental Optometry. 105 (7): 715–720. doi:10.1080/08164622.2021.1973344. PMID 34538220. S2CID 237573319.
- ^ a b c Boyd, Kierstan; Turbert, David (2023-04-29). "Eye Anatomy: Parts of the Eye and How We See". American Academy of Ophthalmology. Retrieved 2023-10-31.
- ^ "Frequently Asked Questions: How do you measure refractive errors?". The New York Eye And Ear Infirmary. Archived from the original on 2006-09-01. Retrieved 2006-09-13.
- ^ "NETRA: Inverse Shack-Hartmann Wavefront Sensor using High Resolution Mobile Phone Display". Vitor F. Pamplona, Ankit Mohan, Manuel M. Oliveira, Ramesh Raskar. Archived from the original on 2011-12-21. Retrieved 2011-12-13.
- ^ Schiefer, Ulrich; Kraus, Christina; Baumbach, Peter; Ungewiß, Judith; Michels, Ralf (2016-10-14). "Refractive errors". Deutsches Ärzteblatt International. 113 (41): 693–702. doi:10.3238/arztebl.2016.0693. ISSN 1866-0452. PMC 5143802. PMID 27839543.
- ^ a b "Refractive Errors in Children - American Association for Pediatric Ophthalmology and Strabismus". aapos.org. Retrieved 2023-10-30.
- ^ Adam, Henry (2020-04-02). "Vision Screening". Pediatric Care Online. doi:10.1542/aap.ppcqr.396022. ISSN 2767-6617. S2CID 263605231.
- ^ a b Cochrane, Gillian M.; Toit, Rènée du; Mesurier, Richard T. Le (2010-04-12). "Management of refractive errors". BMJ. 340: c1711. doi:10.1136/bmj.c1711. ISSN 0959-8138. PMID 20385718. S2CID 8240093.
- ^ Wedner, S.; Masanja, H.; Bowman, R.; Todd, J.; Bowman, R.; Gilbert, C. (2008-01-01). "Two strategies for correcting refractive errors in school students in Tanzania: randomised comparison, with implications for screening programmes". British Journal of Ophthalmology. 92 (1): 19–24. doi:10.1136/bjo.2007.119198. ISSN 0007-1161. PMID 18156372. S2CID 2157969.
- ^ "Pediatric Ophthalmology, Optometry and Orthoptics". Asian Eye Institute. Retrieved 2022-08-03.
- ^ "Eyeglasses for Refractive Errors | National Eye Institute". www.nei.nih.gov. Retrieved 2021-06-29.
- ^ Mukamal, Reena (2023-05-03). "10 Cataract Surgery Side Effects, and How to Cope". American Academy of Ophthalmology. Retrieved 2023-11-06.
- ^ "LASIK — Laser Eye Surgery". American Academy of Ophthalmology. 2023-07-26. Retrieved 2023-11-06.
- ^ Shih, Yung-Feng; Hsiao, C. Kate; Chen, Chien-Jen; Chang, Ching-Wei; Hung, Por T.; Lin, Luke L.-K. (June 2001). "An intervention trial on efficacy of atropine and multi-focal glasses in controlling myopic progression". Acta Ophthalmologica Scandinavica. 79 (3): 233–236. doi:10.1034/j.1600-0420.2001.790304.x. ISSN 1395-3907. PMID 11401629.
- ^ Lee, Jong-Jer; Fang, Po-Chiung; Yang, I-Hui; Chen, Chih-Hsin; Lin, Pei-Wen; Lin, Sue-Ann; Kuo, Hsi-Kung; Wu, Pei-Chang (February 2006). "Prevention of Myopia Progression with 0.05% Atropine Solution". Journal of Ocular Pharmacology and Therapeutics. 22 (1): 41–46. doi:10.1089/jop.2006.22.41. ISSN 1080-7683. PMID 16503774.
- ^ a b Li, X; Friedman, IB; Medow, NB; Zhang, C (1 May 2017). "Update on Orthokeratology in Managing Progressive Myopia in Children: Efficacy, Mechanisms, and Concerns". Journal of Pediatric Ophthalmology and Strabismus. 54 (3): 142–148. doi:10.3928/01913913-20170106-01. PMID 28092397.
- ^ Walline, JJ (January 2016). "Myopia Control: A Review". Eye & Contact Lens. 42 (1): 3–8. doi:10.1097/ICL.0000000000000207. PMID 26513719. S2CID 24069302.
- ^ Kandel H, Khadka J, Goggin M, Pesudovs K (2017). "Patient-reported outcomes for assessment of quality of life in refractive error: a systematic review". Optometry and Vision Science. 94 (12): 1102–1119. doi:10.1097/OPX.0000000000001143. PMID 29095758. S2CID 21512136.
- ^ Kandel H, Khadka J, Lundström M, Goggin M, Pesudovs K (2017). "Questionnaires for measuring refractive surgery outcomes". Journal of Refractive Surgery. 33 (6): 416–424. doi:10.3928/1081597X-20170310-01. PMID 28586503.
- ^ "WHO Disease and injury country estimates". World Health Organization. 2009. Archived from the original on 2009-11-11. Retrieved Nov 11, 2009.
- ^ Hashemi, Hassan; Fotouhi, Akbar; Yekta, Abbasali; Pakzad, Reza; Ostadimoghaddam, Hadi; Khabazkhoob, Mehdi (2017-09-27). "Global and regional estimates of prevalence of refractive errors: Systematic review and meta-analysis". Journal of Current Ophthalmology. 30 (1): 3–22. doi:10.1016/j.joco.2017.08.009. ISSN 2452-2325. PMC 5859285. PMID 29564404.
- ^ "Global Disease Burden of Uncorrected Refractive Error Among Adolescents From 1990 to 2019" (PDF). Archived from the original (PDF) on 2021-06-24. Retrieved 2023-03-21.
- ^ Kuryan J, Cheema A, Chuck RS (2017). "Laser-assisted subepithelial keratectomy (LASEK) versus laser-assisted in-situ keratomileusis (LASIK) for correcting myopia". Cochrane Database Syst Rev. 2017 (2): CD011080. doi:10.1002/14651858.CD011080.pub2. PMC 5408355. PMID 28197998.
